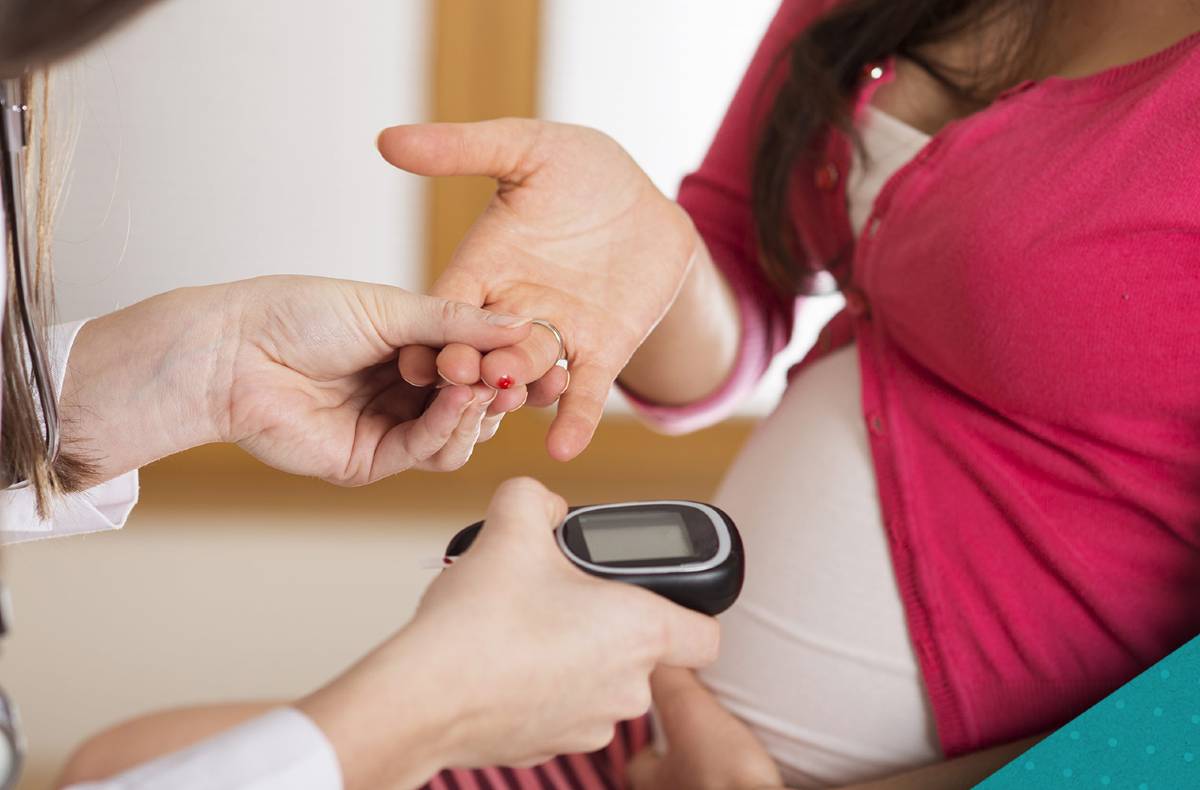
Why are many pregnant women diabetic?
GDM is any glucose intolerance that begins during pregnancy.
the glucose intolerance may have been pre-existing or started during the current pregnancy.
GDM is a common pregnancy condition. It can harm both the mother and the child.
It has been proven that Pregnancy changes maternal glucose metabolism. Placental hormones enhance insulin resistance throughout pregnancy. Insufficient insulin release in response to high blood sugar causes GDM.
GDM screening begins at the time of “booking”. Fasting blood glucose or timed glucose levels are measured and rechecked at 24–28 weeks of gestation with a 75gm oral glucose tolerance test (OGTT). Low-risk pregnant women follow this monitoring protocol. Patients at high risk of GDM in the present pregnancy are screened twice with the 75gm GTT, once during the booking visit and again at 24-28 weeks.
High-risk women are those with
- BMIs of 30 kg/m2.
- Previous GDM or fetal macrosomia.
- Diabetes Mellitus in the family.
- urine dipstick glucose (2+ or above on one occasion, 1+ on two or more times).
Management:
An obstetrician, endocrinologist, and dietitian manage this condition of GDM. As pregnancy progresses, certain patients may need pharmacologic therapy with pills or insulin injections to avert problems.
How does it affect the fetus and the newborn (before and after birth)?
Uncontrolled GDM can harm fetal growth in each trimester.
During the first trimester it may cause spontaneous miscarriages and significant congenital abnormalities. Usually if the diabetes is obvious in these mothers.
Uncontrolled glucose can cause fetal macrosomia (abnormally large fetal growth) and sudden intrauterine death in the second and third trimesters.
Postnatal hypoglycaemia, jaundice, and polycythemia are more likely to babies born to mothers with GDM.
GDM in the mother increases the likelihood of childhood obesity and glucose intolerance.
GDM fades in 95% of women post-delivery. But are the 20%–60% chance of getting diabetes in the future and there is an increased risk of GDM in consecutive pregnancies.
Therefore a 75 gm OGTT (2-step) should be done at least 6 weeks post-partum if glucose levels and OGTT are normal. Lifestyle modification and Annual glucose and HbA1C testing can detect worsening glycemic control and predict Type 2 DM.
All patients with a past history of GDM should consider lifestyle, diet, and exercise regimens to reduce insulin resistance and prevent or delay DM.
If the OGTT is impaired, lifestyle changes and 3–6-month blood glucose monitoring are recommended.
If gestational diabetes continues post-delivery, we start DM treatment with the endocrinologist.
Families should help children adopt an obesity-preventive culture and good habits from a young age to prevent GDM and its adverse effects that can affect the whole life of the mother and child.



